
The cost of prescriptions (Photo: Flickr)
Opinion: Reforming Pharmacy Benefit Managers Will Improve Drug Affordability
Congress must do more to reform the broken policies PBMs enforce
By Beth Smith, August 1, 2023 3:37 pm
Medically vulnerable patients in Nevada and across the country can face extraordinary challenges accessing and affording their prescribed treatments. That is particularly true for cancer patients and those living with immunodeficiency diseases and deficiencies.
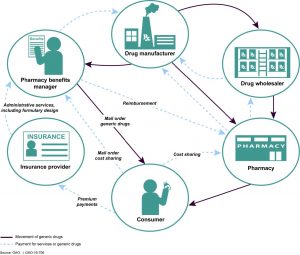
Unfortunately, a large part of the reason we face such high barriers to care is due to the problematic policies of little-known healthcare players called “Pharmacy Benefit Managers” (PBMs). While some see these PBMs as ‘Superman’, as an opinion piece that ran on July 21 says, these shadowy organizations are actually hiding behind a mask, operating with little transparency and accountability as they dictate what medications people have access to and their out-of-pocket costs.
To improve access and reduce sky-high out-of-pocket costs for patients, Congress must do more to reform the broken policies PBMs enforce. Thankfully in the Senate, there is a bipartisan effort called the Delinking Revenue from Unfair Gouging (DRUG) Act that could help prevent PBMs from price-gouging consumers and even the playing field for patients like me.
Unfortunately, I speak from experience on this issue having been diagnosed with primary immunodeficiency deficiency (PI) in 2019 and Hodgkin Lymphoma just last fall. The medication I take to help build my immunity costs about $70,000 annually and, even with insurance through my employer, I face out-of-pocket expenses.
The entire process was eye-opening—and not in a good way. It was incredibly frustrating, for example, to see the struggles immunologists go through to get insurance approvals for their patients and keep those approvals.
Often, insurers and their associated PBMs will require patients with immunodeficiency diseases to stop taking their prescribed medications and undergo new lab work just to prove they still need it. This interruption in care can result in patients getting serious, life-threatening infections or even suffering organ failure—all in the name of cutting costs.
Nationally, anywhere from 35,000 to 50,000 Americans are estimated to be dependent on medications to treat PI. Known as immunoglobulin replacement therapy, these treatments work to replace the antibodies that the body cannot make on its own. Just like cancer treatments, these medications can cost tens of thousands of dollars a year.
That makes it all the more upsetting to know that insurers and PBMs also play a major role in keeping out-of-pocket expenses for vital prescription drugs higher than they should be. While PBMs work with drug manufacturers to negotiate discounts on prescription medications, they rarely pass any of these savings down to patients by counting them toward their insurance deductibles and out-of-pocket expenses.
Instead, PBMs are able to simply keep these savings for themselves, increasing their profits to the detriment of patients who must struggle to pay higher out-of-pocket costs for the medications, treatments, and therapies they need. Something has to change.
Fortunately, legislation at the national level like the DRUG Act would address this issue by reforming the many policies PBMs use to put their own profits over the wellbeing of vulnerable patients. Senator Rosen and Senator Cortez Masto should follow suit of their democratic colleagues in the Senate to support this legislation to help increase access and improve affordability for patients with cancer, immune deficiencies, and a range of other conditions by passing this much-needed legislation.





I buy prescription drugs in Algondones MX with out a prescription- allowed 90day supply of non narcotics drugs under NAFTA